This is an explanation of my eye conditions which accompany blog entries that document what I have learned while adapting to changes in my vision. As well as low vision and more recently blindness as defined by MSD I also have hearing loss and in the last five years have identified as deafblind.
Background …
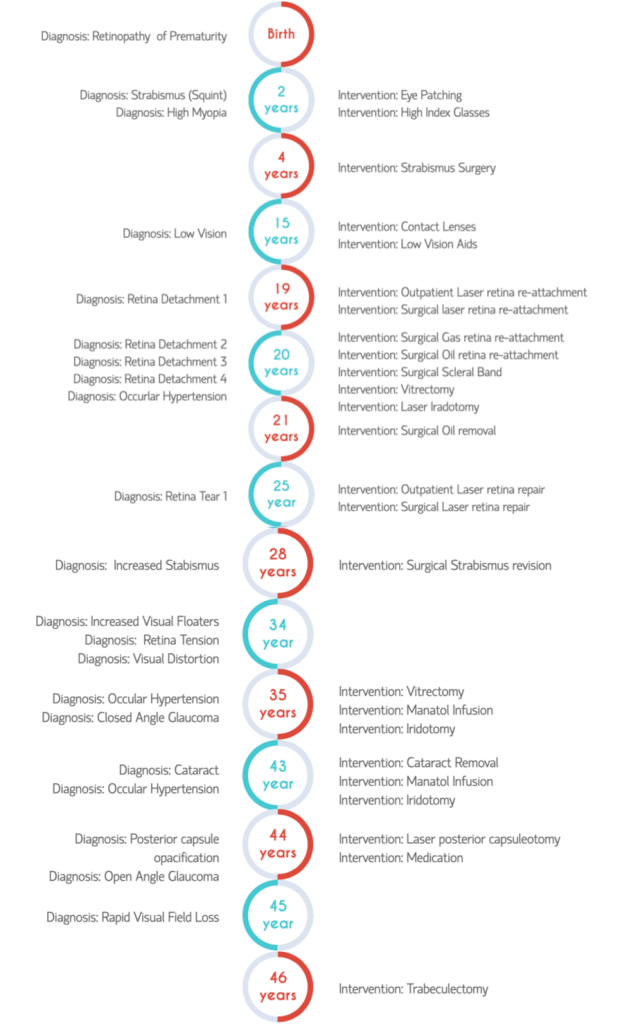
I was born earlier than I should have been (expected in late April / early May but born in early February), I spent over three months in neonatal intensive care and treatments there along with premature birth caused me to have retinopathy of prematurity (ROP). This meant the retina in both of my eyes did not form correctly causing poor vision and I was extremely myopic with a very high negative prescription. The high myopia means that I have a very elongated eyeball and in turn very narrow angles in my eye causing closed angle glaucoma. Over the years, I have had my fair share of eye surgery to get the best vision I can, (I think the current count is around eight or nine surgeries) for various things, including multiple open retina reattachments, a vitrectomy to remove floaters, multiple strabismus corrections, cataract removal, intraoccqular lens implant and multiple hospitalisations for high intraoccular pressure.
My Vision …
My right eye is much smaller than the left in size and currently the retina is held in place using a silicon band to take the pressure off the retina and decrease the chance of a further detachment. This eye is painful in bright sunlight and towards the end of each day. My right eye has no functional vision, which means I have monocular vision, and as a result, poor balance, reduced visual field and no depth perception. Using the picture below, the functional vision I have is from the left of the field of view for 5-10 degrees.

My left eye has good central vision, but peripherally this deteriorates, in particular on the nasal side (or midline). This means that I may occasionally miss objects in front or on my right. Using the diagram to the right my field would be from the left side of the immediate field of view for approximately 5 degrees towards the midline. There are also blind spots in my field of vision which may occlude objects (for example whole letters on the eye chart).
To reduce the intraoccqular pressure and keep the retina in place I have had medications and multiple procedures on my left eye. To relieve the pressure in my left eye, I have had a peripheral iridotomy, which came with a side effect, when looking in certain directions bands of glare, ghosting and “sparkles” are visible which are like bright static in my eye. Similarly a side effect after cataract surgery was the need for a posterior capsulotomy. With a history of having a vitrectomy the removal of the entire posterior capsule was not possible which has meant a remnant of the capsule is still attached and floats into my field of view on movement of my head.
As a side effect of all of these things, glare and light sensitivity are an issue for me. When I questioned one of my specialists around this he answered that he wasn’t surprised as I had very blonde looking retina which may account for this. The term blonde fundus refers to less pigmentation in the retina and is often associated with light sensitivity and susceptibility to glare. This means that in bright situations, I loose definition, as an example, imagine a person is standing in front of a window and it is difficult to see facial expression, however, when they are shaded you can see them well.
At night my visual acuity decreases and lights become haloed and move when I blink or move my head.
in 2021 I had a tra trabeculectomy as my eye vision was decreasing ans pressure unable to be controlled by eye drops. This started to leak in July 2023 and was revised again.